Laser-induced thermotherapy (also known as interstitial laser thermotherapy or LITT for short) is a minimally invasive, image-guided procedure. It uses laser energy to heat and destroy specific tissue with high precision. LITT is primarily used to treat epilepsy foci, brain tumors, or other deep-seated changes in the brain.
How does LITT work?
LITT uses targeted heating of tissue using laser energy to ablate and destroy diseased brain tissue (e.g., tumors or epileptogenic zones).
Stereotactic precision
The procedure is performed under general anesthesia. A special technique known as stereotaxy is used to ensure that the laser is positioned with maximum precision. Depending on the situation, either a stereotactic frame, which is attached to the head with four small screws, or a high-precision robot is used. The next step is to perform a computed tomography (CT) scan of the head. Using these images of the head and the stereotactic coordinates, a specialist then calculates the optimal path to the target region in the brain with millimeter precision.
Minimally invasive access
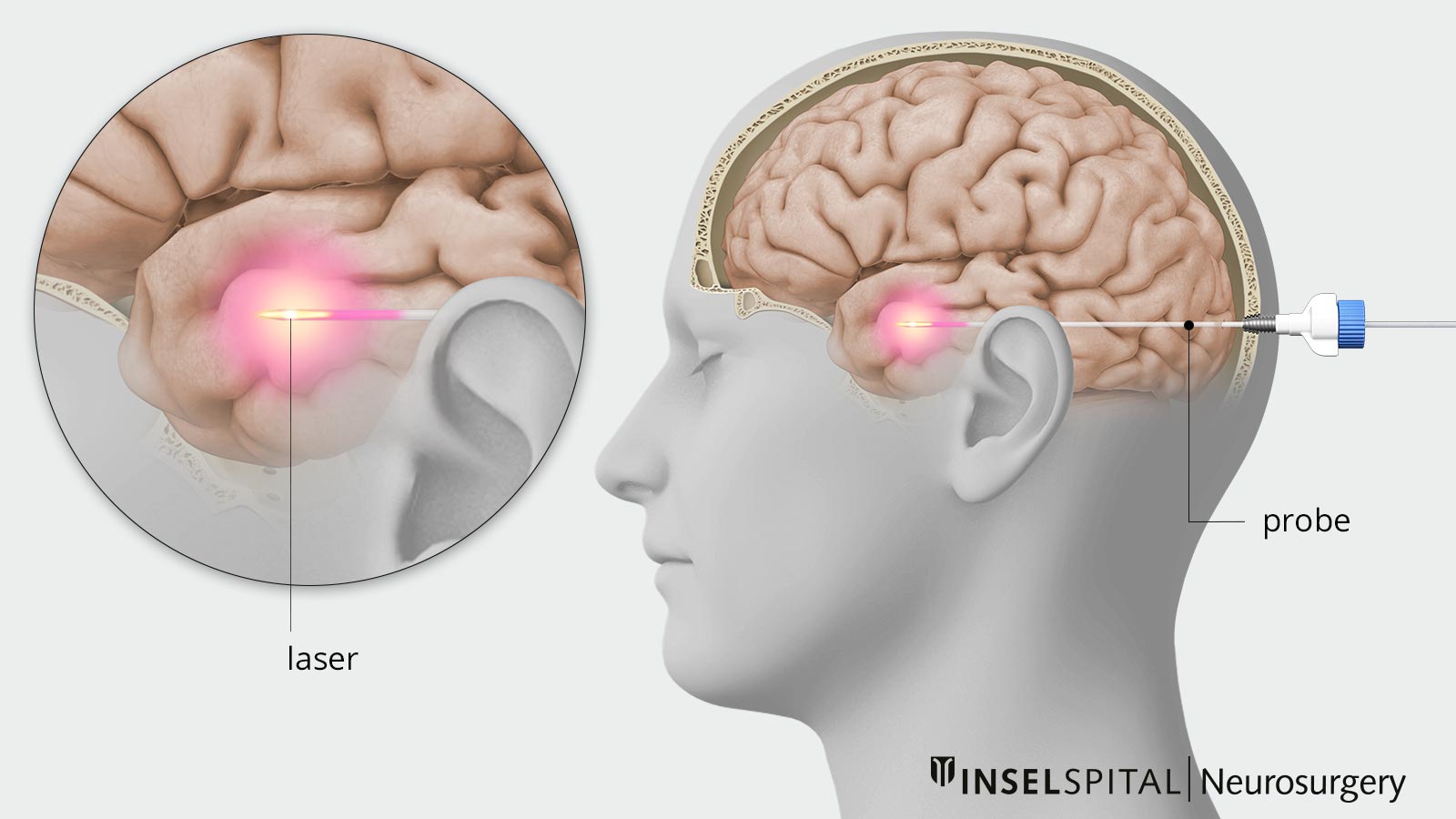
A very thin laser probe is then inserted directly into the affected tissue – for example, into a tumor or a region of the brain that triggers epileptic seizures. The procedure requires only a small incision in the skin and a micro-drill hole just large enough for the probe. This minimizes tissue damage caused by insertion.
Real-time control of the lesion
Laser light is then emitted through the tip of this probe. This light is converted into heat in the tissue. The target tissue is heated to around 50 to 100 degrees Celsius – hot enough to destroy the diseased cells. This process is called thermal destruction or ablation. To ensure that no healthy brain tissue is damaged, the temperature in the brain is closely monitored throughout the entire treatment using a special MRI technique known as thermometry. This shows in real time how hot it is in the area being treated.
In addition, the laser probe has an integrated cooling system that ensures that the heat does not spread unintentionally. This allows the procedure to be performed very precisely and safely.
For which diseases can LITT be used?
LITT is mainly used in neurosurgery and oncology, especially in situations where open surgery would be difficult or risky. Precise planning and imaging are crucial in all cases, as precision is essential to treat the affected tissue and preserve healthy structures.
Common applications in neurosurgery include:
Brain tumors
- High-grade gliomas (e.g., glioblastoma)
- Brain metastases
- Recurrent tumors after radiation or surgery
- Deep-seated or hard-to-reach tumors
- Radionecrosis after radiation therapy
However, not all tumors are suitable for this method: very large or extensive tumors cannot be adequately treated with LITT and must still be removed by open surgery.
Epilepsy surgery
Particularly in cases of drug-resistant focal epilepsy. Here, LITT is used to treat epileptic focus areas, i.e., regions of the brain responsible for seizures. This particularly affects the hippocampus or temporal lobe, where structural changes are often present in drug-resistant epilepsy. A very precise ablation is performed at the target sites to destroy only the cells that cause the seizures.
What are the risks of LITT?
As with any procedure involving the brain, LITT carries certain risks. In rare cases, bleeding, infection, or swelling in the treated tissue may occur. Neurological deficits, such as temporary speech or movement disorders, are also possible, especially if the treated area is located near important areas of the brain.
However, the risk associated with LITT is significantly lower than with open surgery, as the procedure is minimally invasive and very precisely controlled. Before the procedure, a thorough and individual assessment is always carried out to determine whether LITT is the right and safest option.
What are the advantages of LITT?
Laser therapy in the brain (LITT) is a modern, particularly gentle procedure that offers many advantages over conventional surgery—especially when the procedure in the brain needs to be as minimally invasive as possible.
Minimally invasive procedure
Instead of a large opening in the skull, only a tiny drill hole (usually only a few millimeters in size) is required. This means less stress, less pain, and a faster healing process for patients. Usually, only a small stitch remains visible at the site of the micro-burr hole.
Precise treatment
By combining laser and MRI imaging, the diseased tissue can be very precisely localized and treated without unnecessarily damaging healthy surrounding brain tissue.
Short hospital stay
Since the procedure is minimally invasive, only a short hospital stay is often necessary—in many cases, patients can go home after just one to three days.
